Filter
1205
Featured
114
308
Language
Document type
715
170
145
65
39
31
21
8
5
4
1
1
Countries
46
40
38
38
35
32
31
29
20
20
18
16
15
15
15
14
14
13
13
13
13
13
13
12
12
11
11
10
9
9
9
8
8
8
8
8
7
7
7
6
6
5
5
5
4
3
3
3
3
3
3
3
3
3
3
2
2
2
2
2
2
2
2
2
2
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
1
Authors & Publishers
Publication Years
Category
420
110
57
49
44
24
24
Toolboxes
139
119
98
75
69
59
38
35
33
27
23
22
20
16
16
13
13
9
9
9
5
3
1
Recommendations of the Healthcare Infection Control Practices Advisory Committee and the HICPAC/SHEA/APIC/IDSA Hand Hygiene Task Force
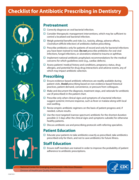
Checklist for Antibiotic Prescribing in Dentistry - Fact Sheet
second edition
Included more self-measured blood pressure (SMBP)-focused content with tools and resources.
Showcased more tools to find patients with potentially undiagnosed HTN.
Added new strategies that focus on chronic kidney
...
Pwoteje Manje ak Dlo Apre yon Dezas oswa Sitiyasyon Ijans
A summary of health effects, resources, and adaptation examples from health departments funded by CDC’s Climate and Health Program
The Mapping Antimicrobial Resistance and Antimicrobial Use Partnership (MAAP) project has conducted a multi-year, multi-country study that provides stark insights on the under-reported depth of the antimicrobial resistance (AMR) crisis across Africa
...
Antimicrobials are medicines, including antibiotics, antivirals, antifungals, and antiparasitics, that are used to prevent and treat infections in humans, animals,
...
AstraZeneca-SKBio in South Korea and Serum Institute of India
Interim guidelines developed by CDC for healthcare providers in the United States caring for infants born to mothers who while pregnant traveled to
...
African Union and the Africa Centers for Disease Control
...
Accessed: 02.04.2020
This policy brief draws from the latest evidence on the impact of vaccination program start date and vaccine rollout rates on health benefits. The objective is to support policymakers on decisions to procure COVID-19 vaccines
...
Event-based surveillance (EBS) is defined as the organized collection, monitoring, assessment and interpretation of mainly unstructured ad hoc information regarding health events or risks, which may represent an acute risk to health. Both indicator-
...
The Core Elements of Outpatient Antibiotic Stewardship provides a framework for antibiotic stewardship for outpatient clinicians and facilities tha
...
Antibiotic stewardship refers to coordinated efforts and activities that seek to measure and improve use of antibiotics. Implementation of ASPs has demonstrated positive public health
...
Los Módulos de autoaprendizaje sobre tuberculosis son una serie de módulos educativos diseñados para proporcionar información sobre la tuberculosis en un formato de autoaprendizaje. El módulo 6 (“Manejo de pacientes con tuberculosis y mejora de la adherencia al tratamiento”) y el módulo 8
...
On January 14-16, 2003, the Centers for Disease Control and
...
This document updates the 2014 Core Elements for Hospital Antibiotic Stewardship Programs and incorporates new evidence and lessons learned from ex
...
The Pocket Guide to Managing Contraceptive Supplies addresses one of
the most important components of any program that provides family
planning services—the logistics system that manages the delivery,
quality, and storage of contraceptive suppl
...
National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention.
Division of Tuberculosis
...
Antibiotics save lives, but poor prescribing practices are putting patients at unnecessary risk for preventable allergic reactions,
super-resistant infections, and deadly diarrhea. Errors in prescr
...
Le cadre de surveillance basé sur les événements est destiné à être utilisé par les autorités et les
agences responsables de la surveillance et de l'intervention. Ce cadre sert de cadre pour guider les
parties prenantes intéressées par la mise en œuvre de la surveillance basée sur le
...
Fason pou Gen Laviktwa sou Kolera
recommended
The document titled "Fason pou Gen Laviktwa sou Kolera" (How to Achieve Victory over Cholera) provides comprehensive guidelines on the clinical presentation and management of cholera, particularly in the context of the 2010 Haiti outbreak. It emphas
...
Dentists are uniquely positioned to play a role in pre enting the spread of antibiotic resistance. Here are se en simple “how-tos” for safe, appropriate antibiotic prescribing and use when treat
...
This Cardiac Rehabilitation Change Package was completed by the Centers for Disease Control and
...
Rete lwen danje apre yon Siklòn
This clinical job aid addresses the importance of maternal health and antiretroviral therapy adherence, as well as care and testing for the HIV-exp
...
Clinical Presentation and Management for Haiti Cholera Outbreak, 2010
National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention
Division of Tuberculosis
...
Evite Maladi Apre Yon Dezas
Evite Blese Apre Yon Dezas
This guide is intended for shelter operators, planners, and staff, as well as emergency managers, public health professionals, and radiation protec
...
This toolkit was developed by the Centers for Disease Control and
...
Antimicrobial resistance (AMR) has emerged as a leading cause of death in the African region, surpassing fatalities from malaria, HIV, and TB. In response to this critical threat, the region has adopted the AMR Global Action Plan
...
A Estrutura de Vigilância Baseada em Eventos deve ser usada por autoridades e agências responsáveis
pela vigilância e resposta. Essa estrutura serve como um esboço para orientar as partes interessadas
em implementar a vigilância baseada em eventos (EBS) usando uma abordagem multissetorial
...
The strategy recommends that AU Member States should enhance, where feasible, existing COVID-19 surveillance to include:
Community-based surveillance to detect symptomatic cases early for treatment
...
Cette note politique s’appuie sur les données les plus récentes concernant l’impact de la date de début du programme de vaccination et des taux de déploiement des vaccins sur les bénéfices pour la santé. L’objectif est de soutenir les décideurs politiques dans leurs décisions d’appr
...
Document available in English, Spanish and French.
Document availablein English, Spanish and French.
Ebola disease and Marburg disease outbreaks continue to occur in Africa, with increased frequency. In addition to resulting in high mortality
...
This document aims to provide guidance to healthcare facilities and healthcare providers in the European Union/European Economic Area (EU/EEA) and the United Kingdom (UK) on preparedness
...
Morbidity and Mortality Weekly Report (MMWR) October 4, 2019 / 68(39);851–854
Infectious disease outbreaks and epidemics are increasing in frequency, scale and impact. Health care facilities can amplify the transmission of em
...
Epidemiology
Chagas disease (American trypanosomiasis) is caused by the protozoan parasite Trypanosoma cruzi, and transmitted to humans by infected triatomine bugs,
...
Interim rapid response guidance, 10 June 2022.
It includes considerations for certain populations such as patients with mild disease with considerations
...
The WHO continuously reviews available data on SARS-CoV-2 variants of concern. For this version, the global epidemiological
situation of the COVID-19 pandemic as of 21 January 2022 – at a time when the Omicron VOC had been identified in 171
coun
...
The Infection prevention and control in the context of coronavirus disease 2019 (COVID-19): a li
...
Noncommunicable diseases (NCDs) such as cancer, cardiovascular disease, diabetes and chronic respiratory diseases and their risk factors are an inc
...
The World Health Organization Regional Office for Africa (WHO AFRO), in accordance with recommendations from various WHO committees, has developed three flagship initiatives to support Member States in the African region to prepare
...
Important Guideline for Ebola prevention and control
It is designed
...
Clinician Outreach and Communication Activity (COCA) Call
April 12, 2016
The purpose of this interim guidance is to provide information and insight to assist public policy and
health system leaders in preparing for
...
The roundtable provided a forum that allowed communicators across a number of Federal agencies to share information, strategies, and challenges in developing and providing communicatio
...
The objective of this document is to guide the preparation and implementation of national preparedness plans for the safety of substances of human origin during outbreaks of Zika virus infection, bo
...
MMWR. Recommendations and Reports:
December 16, 2005 / 54(RR15);49-55
This document updates recommendations for HIV testing by laboratories in the United States and offers approaches for reporting test results to pers
...
The Public Health Burden of Commercial Tobacco Use
The burden of disease and death from commercial tobacco* use in the United States is
overwhelmingly caused by cigarettes
...
The Public Health Burden of Secondhand Exposure to Commercial Tobacco Smoke Secondhand smoke, the combination of smoke from burning commercial tobacco* products and the smoke breathed out by a person who is smoking, is deadly.
Preparedness planning is essential in order to respond effectively to outbreaks, including single case occurrences of highconsequence infectious diseases (HCID), such as the importation of a viral haemorrhagic fever (VHF) case
Euro Surveillance 2014;19(47):pii=20970, p.31-37
The major areas of focus for the plan will be:
- Social mobilization and community empowerment (health promotion & education for ...
- Social mobilization and community empowerment (health promotion & education for ...
Rabies is a fatal viral zoonosis and serious public health problem.1 All mammals are believed to be susceptible to the disease, and
...
Downloaded from https://aidsinfo.nih.gov/guidelines on 10/19/2019
Recommendations from the National Institutes of Health, Centers for Disease Control
...
The Sierra Leone National Infection Prevention and Control Guidelines were jointly developed and
...